Key facts
Tuberculosis – *A total of 1.5 million people died from TB in 2018 (including 251 000 people with HIV). Worldwide, TB is one among the highest 10 causes of death and therefore the leading explanation for one infective agent (above HIV/AIDS).
*In 2018, an estimated 10 million people fell ill with tuberculosis(TB) worldwide. 5.7 million men, 3.2 million women and 1.1 million children. there have been cases altogether countries and age groups. But TB is curable and preventable.
*In 2018, 1.1 million children fell ill with TB globally, and there have been 205 000 child deaths thanks to TB (including among children with HIV). Child and adolescent TB is usually overlooked by health providers and may be difficult to diagnose and treat.
*In 2018, the 30 high TB burden countries accounted for 87% of latest TB cases. Eight countries account for 2 thirds of the entire , with India leading the count, followed by, China, Indonesia, the Philippines, Pakistan, Nigeria, Bangladesh and South Africa .
Tuberculosis (TB) is an infectious disease that harms people’s lungs or different pieces of the body and can cause serious illness and death.
TB is caused by the bacterium (germ) Mycobacterium tuberculosis.
Recent Posts
The difference between active and latent TB disease
People infected with TB bacteria might not get sick because their bodies are ready to repel the infection. this is often called latent or inactive TB, and isn’t infectious.
People who are infected with the TB bacteria that multiplies and grows and therefore the system isn’t ready to repel the bacteria are said to possess active TB. These people will have symptoms and are infectious.
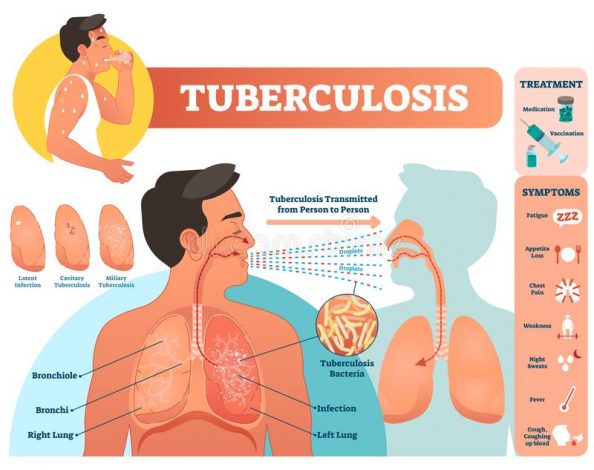
How tuberculosis is spread
TB is spread through the air when a person with active TB disease spreads the bacteria by coughing, sneezing, shouting, speaking or singing and people nearby inhale the bacteria.
High-risk groups of tuberculosis
You are most at risk if you:
*have been recently infected with TB bacteria, including people that work on the brink of someone with active TB, who live in countries where there’s tons of TB, and young children.
*have a medical condition that weakens your immune system , like HIV or AIDS, diabetes and some cancers.

Tuberculosis symptoms
*feel tired and unwell
*have a nasty cough that *lasts a minimum of 3 weeks
*lose weight
*have a fever and sweat in bed at night
*cough up blood within the sputum (phlegm)
*have chest pains
*have swollen lymph glands
Tuberculosis diagnosis
Your doctor may order TB skin and blood tests, sputum tests and chest x-rays.
The results of the tests can take an extended time — 6 weeks or more — to return back.
Tuberculosis treatment
For latent TB your doctor can prescribe tablets to reduce back the danger of you developing active TB.
For active TB, you’ll be prescribed a mixture of special antibiotics, which you must take for at least 6 months.
You may need initial treatment in hospital. If you complete the complete treatment, you’ll be cured of TB disease.Because TB may be a notifiable disease, doctors must report all cases to the health authorities.
Precautions for tuberculosis patients
*Finish the complete course of all TB medicines otherwise you could become seriously ill or die.
*Cover your mouth when coughing or sneezing. Ask family and close contacts to go to their doctor or clinic for TB tests.
Tuberculosis prevention
There is a vaccination against tuberculosis, but it’s not recommended for everybody . The vaccine registered to be used in Australia has not been available for a few time.
Alternative unregistered vaccines could also be available through special prescribing arrangements.
It is recommended for Aboriginal and Torres Strait Islander babies living in some parts of Australia, children who are travelling to parts of the world where there’s tuberculosis, and young children who are exposed to leprosy at home . Everybody is suggested to have a skin test before they are vaccinated.
Tuberculosis vaccine
Vaccination is your best protection against tuberculosis. This table explains how the vaccine is given, who should catch on , and whether it’s on the National Immunisation Program Schedule. Some diseases are often prevented with different vaccines, so ask your doctor about which one is appropriate for you.
Ref – https://www.healthdirect.gov.au/tuberculosis
.

